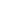The warmer months are when we’re more likely to see and feel the dry bumpy, sandpaper-like skin that flags the skin condition keratosis pilaris. Summer can be an embarrassing time for sufferers, and is when we’re more likely to notice the dry, sometimes itchy and inflamed bumps that resemble chicken skin; although the colder, drier months are when the condition typically worsens in appearance.
If you can answer yes to any of the following questions you’re probably suffering from this common, easily identified, benign skin condition called keratosis pilaris or ‘chicken skin’.
- Do you have skin, which looks perpetually goose-bumped or cold?
- Do you suffer from dry, bumpy skin on your upper arms, thighs or bottom?
- Do the bumps tend to worsen during dry weather?
Don’t get ‘cooped up’, Keratosis pilaris is not infectious or life threatening, just cosmetically displeasing. Whilst there’s no ‘cure all’ for this chronic skin condition, thankfully, there are many treatment options which can relieve the symptoms and help to reduce the appearance.
For some, keratosis pilaris causes sufferers to become extremely self-conscious, continuing to wear winter clothing long into sweltering summer conditions for fear of exposing their chicken skinned bingo wings, to the queuing anonymous behind them at the local supermarket.
If teenage years aren’t difficult enough…..
Keratosis pilaris affects 50-80% of adolescents and commonly presents in puberty, resolving for the majority of sufferers in adulthood. No need to cry ‘fowl’ of this embarrassing condition, ‘cluck’ into action; there are treatment options available!
What is it?
Keratosis pilaris is a common skin condition characterised by rough, dry patches and tiny bumps on the upper arms thighs cheeks or bottom. Keratosis pilaris is a buildup of skin cells called keratin which form a plug, blocking the hair follicle, forming the bump.Sometimes a small hair may be coiled beneath the bump.
Why do we get it?
The origin of keratosis pilaris is unknown but it more frequently affects people with dry skin or sufferers of other skin conditions. It may also be an inherited condition affecting more females than males.
Although there is no known cause there appears to be a strong genetic link; 30-50 % of sufferers have a family history of keratosis pilaris, also people who also suffer with atopic dermatitis, dry skin, asthma and allergies have an increased predisposition.
What can be done-Scratching around for treatment options!
- Avoid cleansers containing sodium lauryl sulfates which may irritate the skin, instead use mild, gentle, non-soap cleansers such as an oil based cleanser.
- Moisturise daily and often where possible.
- Include Alpha Hydroxy Acids in moisturisers to help exfoliate dry skin such as lactic and glycolic acid.
- Use loofahs or mitts to gently exfoliate the affected areas during showering, avoiding if bumps are inflamed.
- If the affected area is inflamed, consider salicylic acid which will help with exfoliation in addition to helping to reduce inflammation – salicylic get levitra pills new is commonly seen in formulation with Urea cream.
- Urea cream is a keratolytic used in helping to breakdown hard, scaly skin.
- Intense Pulsed Light (IPL) and Lasers have also been found to be helpful with improving the overall skin texture and in reducing redness.
Keratosis pilaris “don’ts”
- Don’t use harsh soaps cialis vente libre pharmacie france or cleansers.
- Don’t scrub harshly or try to scrape off the skin especially if the area is inflamed.
- Don’t expect immediate results with topical creams; be patient, diligent and consistent!
- Never give up hope.
In-clinic, I always try to encourage my clients to begin with the ‘KISS’ approach before embarking on expensive alternative treatment options; often the simple treatments result in the best outcomes. Remember, keratosis pilaris is a chronic skin condition requiring patience and long term maintenance for optimal results.
ASkinSolutions x
Do you have any treatment options which have worked, I’d love to hear them?